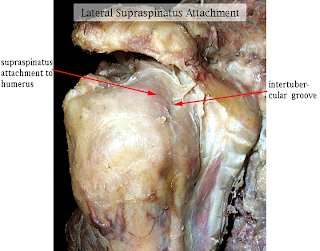
The Scalene Muscle & Potential pain generating factors from scalene

The scalene muscles are a group of three pairs of muscles in the lateral neck, namely the scalenus anterior, scalenus medius, and scalenus posterior. They are innervated by the spinal nerves C3-C8. Origin and insertion Scalenus anterior & medius: Scalenus anterior muscle arises from anterior tubercles of transverse processes of C3-6 vertebrae. It gets inserted into scalene tubercle on the first rib. Scalenus medius arises from posterior tubercles of transverse processes of C2-7 vertebrae. It gets inserted on the superior surface of the first rib behind the groove for subclavian artery. (J.Anat.Soc. India 55 (2) 52-55 2006 52) Function On neck: All 3 scalene muscles produce rotation of the cervical spine to the same side. Maximum stretching of the scalenes should include rotation to the opposite side. (J Orthop Sports Phys Ther. 2002 Oct;32(10):488-96.) On ribcage & respiration: The action of the anterior and middle scalene muscles is to elevate the first rib and rotate the nec...