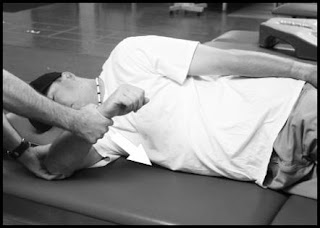
Cadaver study of axial distraction mobilization of the glenohumeral joint support end range mobilization
The axial distraction mobilization techniques are frequently employed for treating patients with joint hypomobility. To know the biomechanical effects 3 different positions of glenohumeral abduction on a fresh cadaveric specimen ware chosen. They are 1. resting position 2. neutral position 3. end-range position Result indicated that displacement of the humeral head ware as follows: 1. largest in the resting position (27.38 mm) 2. followed by the neutral (22.01 mm) 3. and the end range position (9.34 mm). Greater gain in mobility was obtained in distraction at the end range position. During distraction mobilization, the force applied by the therapist and displacement of the humeral head depends on the joint position tested. These results also provide rationales for choosing end range distraction mobilization for improving joint mobility. Reference: Authors: Ar-Tyan Hsuab, Jing-Fang Chiuc, Jia Hao Changd